About the London Transformation and Learning Collaborative Adult Critical Care programme
The London Transformation and Learning Collaborative (LTLC) is a Health Education England and NHS England & Improvement initiative that was established in summer 2020 to support the cross-skilling of the London NHS workforce in response to the Coronavirus pandemic and to prepare for the second surge and beyond.
The LTLC adult critical care programme aims were to broaden the skills base of this workforce to manage existing, and potential future surges in, critical care demand. The programme supported London’s recovery plan by ensuring that:
- training infrastructures could adapt to any future surge and increased critical care capacity
- staff wellbeing for all colleagues was considered
- opportunities for workforce and training innovations were maximised and continually adapted
The development of the LTLC adult critical care programme ended in September 2021, but this programme page and associated pages will remain live on elearning for healthcare (elfh) for the foreseeable future. Keep in touch with the team on Twitter and LinkedIn using the hashtag #NHSLTLC
Please contact the LTLC team for any further information or questions about the programme (ltlc@hee.nhs.uk)
-
Our approach
The aim of the LTLC was to increase the supply and resilience of London’s critical care workforce through:
- the development of a modular education programme that could be tailored to distinct learner needs
- multi-channel delivery of education to accommodate different skill training requirements and enable widespread accessibility
- sharing of practice from critical care units across London (for example, proformas, job descriptions and reports of positive interventions), that other units considered adopting or adapting
- mapping of optimal critical care workforce models in 8 key surge sites, that would inform their learner needs
- incorporation of a feedback mechanism, to refine and evolve the programme’s educational content over time
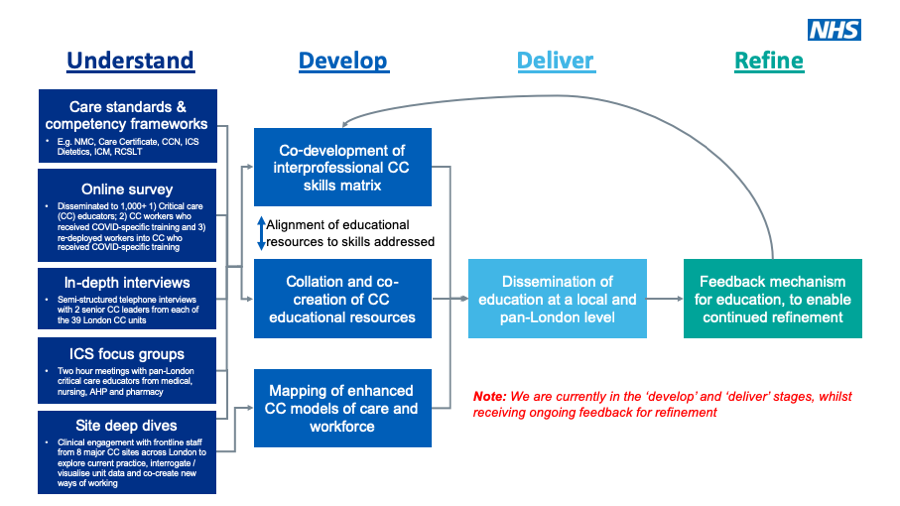
The programme has always been user-led, with both the systems and future learners actively involved in every stage, from development to delivery. We worked with the 5 integrated care systems (ICS) in London to ensure we were responsive to different needs across the capital during the July 2020 to September 2021 stages of the COVID-19 pandemic.
The below chart illustrates the different stages of the programme.
-
Desired outcomes
We have collated educational material for learners and educators that could be tailored to learners’ existing skill level and current, or future, critical care role. These included materials for elearning, face to face teaching, simulation and work-based placements as well as personal development.
We also developed new materials to fill in gaps highlighted by mapping content to the skills matrix. The new materials we developed are showcased on the Rapid Access Resources page.
For learners, we aimed to deliver:
- easy identification of required and desired skills aligned to your current role or expected critical care role
- materials for self-directed learning, resources, and work-based placements to improve confidence and competence working in critical care (including for COVID-19 specifically)
For trainers, we aimed to deliver:
- easy identification of required and desired skills aligned to your learners’ current role or expected critical care role
- efficient collation, design and delivery of educational content and train-the-trainer materials to cross-skill the critical care workforce (including for COVID-19 specifically)
-
Other LTLC programmes
Since the Coronavirus pandemic, the LTLC has been responsible for the rapid and responsive co-development of a number of national cross-skilling programmes that aim to increase the capacity and capability of the workforce in response to urgent needs and demands of the healthcare system through the curation and development of free, open-access, interprofessional educational resources.
-
Meet the team
- Julie Combes, Programme Lead
- Lydia Lofton, Governance and Implementation Lead
- Kathy Brennan, Governance and Implementation Lead
- Libby Thomas, Education Lead
- Ella Nuttall, Project Management Office (PMO) Lead
Education Content Curation & Design- Becky Kay, Healthcare Science
- Cecily Borgstein, Occupational Therapy
- Clare Leon-Villapalos, Nursing
- Dereck Gondongwe, Pharmacy
- Emma Priestley, Nursing
- Lliam Edger, Medicine
- Lucy Brock, Physiotherapy
- Nicola Dover, Nursing
- Ruth McCabe, Medicine
- Claire Wroe, Adult Digital Skills Passport Clinical Lead
Project Management Office- Emma Harper, Communications Manager
- Irene Maposa, Project Manager
- Fatema Limbada, Project Manager
- Simon Munns, Project Manager
- Christine Strickett, Support Officer
- Rani Mehmi, Support Officer
Integrated Care System (ICS) Teams- Alison Dear, NEL ICS Lead
- Emma Clarey, SWL ICS Lead
- Diane Whyte, NCL ICS Co-Lead
- Walter Burog, NCS ICS Co-Lead
- Jenny Ekstrom, NWL ICS Lead
- Colette Laws-Chapman, SEL ICS Lead
- Vicki Newport – NWL ICS Lead and London Critical Care Digital Skills Implementation Lead
elearning for healthcare (elfh) Team- Frankie O’Brien, elfh Project Manager
- Bob Smith, elfh Platform Delivery Lead
- Louise Garrahan, elfh Communications Officer
- Cathryn Fowkes, elfh digital content support
COVID-19 Surge 2021 – Rapid Access Resources and Staff Recovery Resources
 COVID-19 Surge 2021 – Rapid Access Resources
COVID-19 Surge 2021 – Rapid Access Resources
The LTLC has collated a range of key resources to help individuals, educators and systems prepare and to support NHS staff being deployed for the Coronavirus response. We recognise staff are very busy, so these resources are purposely designed to be short and read/watched on the move or on the ward and include: a searchable equipment support tool, a 360 ICU Orientation for new staff and the RSC and NRSS Passports for surge staff.
 Staff Recovery Resources
Staff Recovery Resources
These resources have been created to support healthcare staff recovering from the COVID-19 pandemic. Not all people approach wellbeing by the same means; these resources acknowledge those differences and cover a variety of approaches, including Developing Wellbeing Conversations, Spaces for Listening, and Creative Story Telling.
How to use this programme
Step 1: Download and use the Interprofessional skills matrix to:
- understand the key skills for working in critical care for your professional role mapped against national frameworks, for example, The Nursing and Midwifery Council (NMC), General Medical Council (GMC)
- identify any skill gaps or skills you would like to learn more about
- find educational resources for these specific skills
Step 2: Explore the multimedia resources for learners and/or trainers:
- Learner: resources for self-directed learning, mapped to skills in the interprofessional skills matrix, split by professional groups and sub-categories. Track which resources you have completed, partially completed or are yet to complete
- Trainer: resources, mapped to skills in the interprofessional skills matrix, split by skills categories and sub-categories. Consider pointing your learners in the direction of the Adult critical care digital skills passports, to prepare in advance for future surges
-
How to access
In order to access the LTLC programme, you will need an elfh account. If you do not have one, then you can register by selecting the Register button below.
To view the LTLC programme, select the View button below. If you already have an account with elfh, you will also be able to login and enrol on the programme from the View button.
Registering large numbers of users
If you are a HR, IT or Practice Manager and would like to register and enrol large numbers of staff within your organisation for access onto the LTLC programme, please contact elfh directly.
More information
Please select the following link for more information on how to use the elfh Hub.
Interprofessional skills matrix (Step 1)
We have developed a skills matrix that maps the most useful educational content to the skills they address, by professional group or role within critical care, and for learners and trainers. The content is matched against NMC, GMC, The Health and Care Professionals Council (HCPC), The Critical Care National Network Nurse Leads Forum (CC3N) and Competency-Based Training in Intensive Care Medicine in Europe (CoBaTrICE) professional competencies to aid presentation for revalidation and appraisal.
Download the ![]() (Microsoft Excel, 194KB)
(Microsoft Excel, 194KB)
The searchable equipment training matrix is available under ‘Generic Skills (includes Safety, Communication, Wellbeing, Human factors)’ either below, or via the elfh Hub.
-
About the skills matrix
About the skills matrix
The matrix includes recommended skills for the following posts:
- ICU Generic Skills: for all staff members deployed to work in ICU. These are the basic requirements
- COVID-19 Generic Skills: for all staff members working within a COVID-19 area
- NRSS (non-registered support staff): for all staff who are not registered under a professional body
- RSC (registered support clinician): for all staff who are registered under a professional body (for example, NMC, GMC, HCPC). They may be redeployed to critical care areas during surge or caring for patients on wards who are more unwell than usual (deteriorating/ICU step down). These learning outcomes have all been mapped where possible to the CC3N Step 1 competencies (National Clinical Framework for Registered Nurses (NCFRN) for Adult Critical Care Nurses Critical Care Networks National Nurse leads (CC3N) Step 1 competencies)
- PT (physiotherapist): for physiotherapists with minimal or no previous ICU experience (skills matrix in early stages of development – significant revision required)
- OT (occupational therapist): for occupational therapists with minimal or no previous ICU experience (skills matrix in early stages development – significant revision required)
- SLT (speech and language therapists): for speech and language therapists with minimal or no previous ICU experience (skills matrix in early stages of development – significant revision required)
- Dieticians: for dieticians with minimal or no previous ICU experience (skills matrix in early stages of development – significant revision required)
Note: AHP roles may vary depending on local workforce planning. The skill matrix focusses on cross-skilling non-critical care specialist AHPs to be competent in working within ICU, undertaking tasks that will allow experience critical care AHPs and other team members to deliver more complex tasks requiring more extensive training.
- HCS (Healthcare Scientists): skills matrix in early stages of development – significant revision required
- Pharmacy (Pharmacists): not yet available
- Surge Doctor: 1. doctors who have had minimal (less than 3 months) or no previous ICU experience OR 2. non-critical care doctors who have had more than 9 months of critical care experience. They may be redeployed to critical care areas during surge or caring for patients on wards who are more unwell than usual (deteriorating/ICU step down). These learning outcomes have all been mapped to help learners track their self-development to their own training and revalidation needs as appropriate. Curricula mapped to are:
– Competency Based Training in Intensive Care Medicine in Europe competencies (CoBaTRice)
– Faculty of Intensive Care Medicine (FICM) Core and Common competencies (which map against ACCS, CAT and CMT competencies)
– GMC Good Medical Practice (GMP)
The skills matrix has been created to assist with cross skilling staff in preparation for ICU bed expansion. The skills and learning objectives are taken from national frameworks for individual professional bodies. If a skill falls under a particular competency framework, this has been mapped on the matrix. This is not a prescription of the skills to be undertaken by each role, they are recommendations as to what essential and priority skills are deemed to be necessary to allow flexibility within an ICU team but with precedence on safe patient management. It is not designed to limit a professional scope. The intention is to cover the key interventions and therapies available within intensive care; any additional specialised intervention and therapies may be beyond the scope of this matrix. The skills and roles will require adaptation to local workforce and care remodelling. The skills are suggestions as to what we feel should be delivered with the delivery being undertaken by local teams.
-
How to use the skills matrix
How to use the skills matrix
- Download and open the matrix using the link above
- Select the correct tab:
– “ICU Generic skills” and “COVID-19 Generic skills” tabs: Skills relevant for all professional groups
– Remaining tabs: Skills relevant for specific professional groups (for example, registered support clinician, physiotherapist)
– For detailed descriptions of each professional group, click on the first tab “Introduction to skills matrix” - Identify skills of interest: in each tab skills have been written at 3 levels of depth, to support you to identify your gaps or areas for improvement:
– Category (for example, “Safety”)
– Sub-category (for example, “Infection prevention and control”)
– Learning objectives (for example, “Infection control in ICU including ETT, disposing of fluids from filters / suction cannisters, sending investigations to lab”)
– We recommend downloading the skills matrix document and marking the skills of interest you have identified - Identify relevant resources: once you have identified skills that you want to know more about you can find relevant educational resources in the “Learner resources” column
- Consider completing the Digital Skills Passport if you are potentially going to be deployed to a critical care unit, as either a registered support clinician (RSC) or non-registered support staff (NRSS), to be prepared and tailor your learning in case another surge happens.
Educational resources for learners (Step 2)
The current educational resources available for learners can be found below. These have been mapped to the skills matrix by professional grouping. We are still in the resource collation and co-creation phase and would appreciate you sharing any relevant resources (please see the below ‘How to give your feedback’ section).
Generic Skills (includes safety, communication, wellbeing, human factors) and COVID-19 Generic Skills are the basic skills required by all healthcare professionals working in the critical care and/or COVID-19 environments. Additional skills and resources are described in the individual professional grouping sections.
-
Generic Skills (includes Safety, Communication, Wellbeing, Human Factors)
For all staff members deployed to work in ICU. These are the basic requirements.
Safety
- Bedside patient safety checks
- Medical Gas Safety
- Infection prevention & control
- Cardiac arrest
- Debriefing
- Local induction
Communication
Documentation
Moving and Handling
Professional Development
Human factors
- Teamwork followership
- Teamwork: MDT
- Teamwork leadership
- Human factors: handover
- Human factors: decision making
- Human factors: assertiveness
- Human factors: escalation
- Human factors: risk management
- Human factors: stress and resilience
Wellbeing
ICU Generic Resources
 Searchable equipment support resource
Searchable equipment support resourceThis mobile-friendly web app allows the user to rapidly access quick guides, manuals and training videos for most of the equipment used in critical care units (paediatric and adults). You can search by equipment purpose, make and model to find specific guides that are all free and open access. It can be added to your mobile device home screen as an app, just follow the instructions when you open it.
Please note, while these are the most accessible guides available, some may not be from manufacturers, and all should be viewed in the context of local trust or site practice.
-
COVID-19 Generic Skills
For all staff members working within a COVID-19 area.
Safety
Communication
COVID-19 Generic Resources
-
RSC (registered support clinician) – staff who are registered under a professional body (e.g. NMC, GMC, HCPC)
An RSC may be:
- a junior ICU nurse who has not yet achieved their step 1 competencies in the National Competency Framework,
- a registered nurse, who works outside of ICU or
- a registered (non-nursing) health care professional.
The RSC may be redeployed to critical care areas during surge or caring for patients on wards who are more unwell than usual (deteriorating/ICU step down). These learning outcomes have all been mapped where possible to the CC3N Step 1 competencies (National Clinical Framework for Registered Nurses (NCFRN) for Adult Critical Care Nurses Critical Care Networks National Nurse leads (CC3N) Step 1 competencies).
To accompany these resources a “skills passport” has been developed to highlight the most important skills for the Registered Support Clinician to hold before starting work on a critical care unit (as identified by senior critical care nurses and educators across London). This skills passport can be accessed digitally for NHS London staff or a Microsoft Word version and both contain:
- An introduction to the passport
- Passport Assessment tool for RSC Staff
- Statement of Competence – to be completed by RSC and supervisor
- Links to elfh resources identified to help achieve RSC status if needed
Safety
Airway
- Endotracheal tube care
- Mouth care (for intubated and non-intubated patients)
- Mouth care (for intubated patients)
- Tracheostomy care
- Airway essential
Breathing
- Respiratory physiology
- Ventilator management
- Chest drain management
- Non-invasive ventilation
- Weaning from ventilation
- Additional therapy
- Oxygen therapy – step down specific
Circulation
- Arterial line management
- Central venous catheter management (inc. care bundle)
- Fluid prescription
- Fluid administration
- Fluid balance
- 12 lead ECG
GI
- Insertion of NGT in sedated/unsedated/ventilated/non ventilated patient
- Dysphagia and oral feeding
- Administration and troubleshooting of NG feed
Neurology
Medication
- Administration of drugs nasogastrically – Content required: please see section below on How to give your feedback and share resources
- Administration of IV therapy
- IV drugs – preparation / administration or prescription – Content required: please see section below on How to give your feedback and share resources
- IV infusions – preparation / administration / management of infusion device or prescription – Content required: please see section below on How to give your feedback and share resources
- VTE thromboprophylaxis
- GI prophylaxis
- Glycaemic control
Assessment, Monitoring and Interpretation
- Taking and recording of vital signs
- Systematic nursing patient assessment
- Observation chart step down
- Electrolyte abnormalities
- Waveform recognition and escalation – Content required: please see section below on How to give your feedback and share resources
- Renal replacement therapy
- Renal physiology – Content required: please see section below on How to give your feedback and share resources
Equipment
- Ventilator management
- Waveform recognition and escalation
- IV infusions – preparation / administration / management of infusion device or prescription
Bedside and patient hygiene
EOL care
Rehabilitation
Transfer
-
NRSS (non registered support staff) – staff who are not registered under a professional body
An NRSS may be:
- a Health Care Support Worker or
- a non-registered member of staff specifically recruited to ICU in this role
- healthcare students who may wish to work on Critical Care Units during the surge as bank staff
The NRSS may be redeployed to critical care areas during surge or caring for patients on wards who are more unwell than usual (deteriorating/ICU step down).
To accompany these resources a “skills passport” has been developed to highlight the most important skills for the Non-Registered Support Staff member to hold before starting work on a critical care unit (as identified by senior critical care nurses and educators across London). This NRSS skills passport document contains:
- An introduction to the passport
- Passport Assessment tool for RSC Staff
- Statement of Competence – to be completed by NRSS and supervisor
- Links to elfh resources identified to help achieve NRSS status if needed
Safety
Airway
- Mouth care (for intubated and non-intubated patients)
- Mouth care (for intubated patients) – Content required: please see section below on How to give your feedback and share resources
- Airway essential
Breathing
Circulation
GI
Neurology
Assessment, Monitoring and Interpretation
- Taking and recording of vital signs
- Systematic nursing patient assessment
- Observation chart ICU
- Observation chart step down
- Renal replacement therapy
Bedside and patient hygiene
EOL care
Rehabilitation
Admission
Transfer
Example of duties
-
PT (physiotherapist)
For physiotherapists with minimal or no previous ICU experience.
Safety
Airway
- Endrotracheal tube care
- Mouth care (for intubated and non-intubated patients)
- Tracheostomy care
- Tracheostomy weaning
- Airway essential
Breathing
- Respiratory physiology
- Ventilator management
- CXR interpretation
- Non-invasive ventilation
- Chest drain management
- Weaning from ventilation
- Additional therapy
- Oxygen therapy – step down specific
Circulation
- Arterial line management
- Central venous catheter management (inc. care bundle)
- Fluid prescription
- 12 lead ECG
GI
Neurology
Medication
Assessment, Monitoring and Interpretation
- Taking and recording of vital signs
- Systematic patient assessment
- Observation chart (ICU)
- Arterial blood gas interpretation
- Respiratory assessment
Equipment
- Ventilator management
- IV infusions – preparation / administration / management of infusion device or prescription
Bedside and patient hygiene
EOL care
Rehabilitation
Moving and Handling
-
OT (occupational therapists)
For occupational therapists with minimal or no previous ICU experience.
Safety
Airway
- Intubation and/or reintubation
- Endotracheal tube care
- In-line suctioning
- Mouth care (for intubated and non-intubated patients)
- Tracheostomy care
- Airway essential
Breathing
- Ventilator management
- Chest drain management
- Non-invasive ventilation
- Weaning from ventilation
- Oxygen therapy – step down specific
Circulation
GI
Neurology
Assessment, Monitoring and Interpretation
Equipment
- Ventilator management
- IV infusions – preparation / administration / management of infusion device or prescription
Rehabilitation
Moving and Handling
Bedside and patient hygiene
-
SLT (speech and language therapists)
For speech and language therapists with minimal or no previous ICU experience.
Safety
Airway
- Mouth care (for intubated and non-intubated patients)
- Tracheostomy care
- Tracheostomy weaning
- Airway essential
Breathing
- Respiratory physiology
- Ventilator management
- Non-invasive ventilation
- Oxygen therapy – step down specific
Circulation
GI
- Insertion of NGT in sedated/unsedated/ventilated/non ventilated patient
- Dysphagia and oral feeding
- Administration and troubleshooting of NG feed
Neurology
Equipment
- Ventilator management
- IV infusions – preparation / administration / management of infusion device or prescription
Bedside and patient hygiene
EOL care
Rehabilitation
-
ODP (operating department practitioner)
For Operating Department practitioners with minimal or no ICU experience.
Safety
Airway
- Endotracheal tube care
- Mouth care (for intubated and non-intubated patients)
- Mouth care (for intubated patients)
- Trachesotomy care
- Airway essential
Breathing
- Respiratory physiology
- Ventilator management
- Non-invasive ventilation
- Additional therapy
- Oxygen therapy – step down specific
Circulation
- Arterial line management
- Central venous catheter management (inc. care bundle)
- Fluid prescription
- Fluid administration
- Fluid balance
- 12 lead ECG
GI
- Insertion of NGT in sedated/unsedated/ventilated/non ventilated patient
- Dyspagia and oral feeding
- Administration and troubleshooting of NG feed
Neurology
Medication
- Administration of IV therapy
- IV drugs – preparation / administration or prescription
- IV infusions – preparation / administration / management of infusion device or prescription
- VTE thromboprophylaxis
- GI prophylaxis
- Glycaemic control
Assessment, Monitoring and Interpretation
- Taking and recording of vital signs
- Systematic nursing patient assessment
- Electrolyte abnormalities
- Renal replacement therapy
Equipment
- Ventilator management
- Waveform recognition and escalation
- IV infusions – preparation / administration / management of infusion device or prescription
Bedside and patient hygiene
EOL care
Rehabilitation
Transfer
-
Dieticians
For dieticians with minimal or no previous ICU experience.
Safety
Airway
Breathing
Circulation
- Arterial line management
- Central venous catheter management (inc. care bundle) (in development)
- Fluid balance
GI
- Insertion of NGT in sedated/unsedated/ventilated/non ventilated patient
- Administration & troubleshooting of NG feed
Neurology
Medication
Assessment, Monitoring and Interpretation
Equipment
- Ventilator management
- IV infusions – preparation / administration / management of infusion device or prescription
EOL care
Rehabilitation
-
HCS (healthcare scientists)
Healthcare scientist (HCS) as a title encompasses a very varied workforce who work in departments from pathology to radiotherapy, through to sleep studies and data analytics. In response to the first COVID surge HCS performed many different roles and had a whole host of responsibilities outside of BAU.
HCS were redeployed as ICU tech support, clinical engineering support, bedside buddies and floating clinical team (at NHS London Nightingale Hospital).
HCS Surge Roles (PDF, 882KB) offers a brief introduction to how HCS could add value in a surge situation
Medical Equipment safety and QA HCS role (PDF, 547KB) provide some details regarding this final role.
Most trusts have a lead HCS who can help identify HCS staff and aid in establishing where their skills could be best utilised.
Equipment
Safety
-
Pharmacy (pharmacists)
Safety
Airway
Breathing
Circulation
- Arterial line management
- Central venous catheter management (inc. care bundle)
- Intravenous vasocative drugs
- Fluid administration
- Fluid balance
GI
Neurology
- Monitoring, managing and weaning sedation
- Glasgow coma score
- Pain management
- Delirium recognition and management
- RASS & CPOT pain scores
Medication
- Respiratory system
- Central nervous system
- Infections
- Endocrine system
- Eye
- Anaesthesia
- Renal impairment
- Parenteral therapy
- Toxicology
- Haemostasis and thrombosis
- Medicine supply
- Medicines reconciliation and de-prescribing
Palliative and EOL care
Transfer
-
Surge Doctor
1. doctors who have had minimal (less than 3 months) or no previous ICU experience OR 2. non critical care doctors who have had more than 9 months of critical care experience. They may be redeployed to critical care areas during surge or caring for patients on wards who are more unwell than usual (deteriorating/ICU step down). These learning outcomes have all been mapped to help learners track their self-development to their own training and revalidation needs as appropriate. Curricula mapped to are:
– Competency Based Training in Intensive Care Medicine in Europe competencies (CoBaTRice)
– Faculty of Intensive Care Medicine (FICM) Core and Common competencies (which map against ACCS, CAT & CMT competencies)
– GMC Good Medical Practice (GMP)Safety
Airway
- Intubation and/or reintubation
- Endrotracheal tube care
- In-line suctioning
- Tracheostomy care
- Airway essential
Breathing
- Chest drain insertion (Seldinger and tube thoracostomy)
- Non-invasive ventilation
- Ventilator management
- Weaning from ventilation
- CXR interpretation (expected to be prior knowledge for all doctors)
- Chest drain management
Circulation
- 12 lead ECG
- Arterial line insertion
- Arterial line management
- Central venous catheter management (inc. care bundle)
- Fluid prescription
- Intravenous vasoactive drugs
- Fluid balance
GI
Neurology
- Monitoring, managing and weaning sedation
- Glasgow coma score
- AVPU
- Delirium recognition and management
- Pain assessment in awake patients
- RASS & CPOT pain scores
Medication
- Antimicrobials
- IV infusions – preparation / administration / management of infusion device or prescription
- VTE thromboprophylaxis
- GI prophylaxis
Assessment, Monitoring and Interpretation
- Taking and recording of vital signs
- A to E assessment
- Critical care patients – full assessment
- Hypoglycaemia and management
- Electrolyte abnormalities
- Waveform recognition and escalation
- Arterial blood gas interpretation
- Renal replacement therapy
Moving and Handling
Bedside and patient hygiene
EOL care
- Completing respect forms/DNAR
- End of life prescription
- Last offices
- Symptom control
- End of life care
- Chaplaincy
Documentation
Transfer
Redeployment
This Surge Doctor Redeployment Suggestions document provides suggestions compiled by the LTLC for supporting the training and well-being doctors being redeployed into critical care. This method allows opportunities for ongoing training and to give appropriate support to critical care as and when the surge need arises. It is up to individual Trusts to determine the exact arrangements that best support patient care. Any redeployments will require the specific approval of the Postgraduate Dean (or nominated deputy).
Adult Critical Care Digital Skills Passports
The LTLC adult critical care digital skills passports are endorsed by the Intensive Care Society, British Association of Critical Care Nurses (BACCN) and Critical Care Network National Nurse Leads Forum (CC3N) and have been developed:
- to support staff to understand, document and acquire new skills to support the safe delivery of critical care (levels 1, 2 and 3) to adults in a surge model of care
- for managerial staff overseeing these surge model roles to have visibility of their team members’ skillsets and capability
The adult critical care digital skills passports can be accessed via mobile, tablet and desktop and have been created for:
- non-registered support staff (NRSS) (for example a health care support worker or a non-registered member of staff specifically recruited to ICU in this role or healthcare students who may wish to work on critical care units during the surge as bank staff
- registered support clinician (RSC) (for example a junior ICU nurse who has not yet achieved their step 1 competencies in the national competency framework, a registered nurse, who works outside of ICU or a registered (non-nursing) healthcare professional)
Resources from the LTLC adult critical care programme have been mapped to the passports’ skill domains to support self-directed learning.
Knowledge Checker for RSC Skills Passport
 This Knowledge Checker is designed to help registered healthcare professionals preparing for deployment to critical care assess their core knowledge on elements of patient care as covered in the RSC Skills Passport. This knowledge and these skills should allow them to slot into the bedside patient care role in critical care with increased confidence. Each element of the passport is covered in the Knowledge Checker and links are provided to free education resources for each question to support further understanding where needed. (under 30 mins to complete, no pass / fail)
This Knowledge Checker is designed to help registered healthcare professionals preparing for deployment to critical care assess their core knowledge on elements of patient care as covered in the RSC Skills Passport. This knowledge and these skills should allow them to slot into the bedside patient care role in critical care with increased confidence. Each element of the passport is covered in the Knowledge Checker and links are provided to free education resources for each question to support further understanding where needed. (under 30 mins to complete, no pass / fail)
CapitalAHP C3Framework
 The CapitalAHP Critical Care Competency framework (C3Framework) has been created to support the professional development of AHPs new to critical care and aid workforce planning of critical care services. More information about its rationale and methodology can be found in this short paper (PDF, 209KB).
The CapitalAHP Critical Care Competency framework (C3Framework) has been created to support the professional development of AHPs new to critical care and aid workforce planning of critical care services. More information about its rationale and methodology can be found in this short paper (PDF, 209KB).
Visit the CapitalAHP C3Framework website to access and download the framework and its supporting materials, including supervised learning events logs and templates. There is ongoing work to implement and improve the framework. Contact details can also be found on the website.
Educational resources for trainers (Step 2)
The current educational resources and train-the-trainer materials can be found below. These have been mapped to the skills matrix by professional grouping. These have been re-organised for ease of access. Your feedback on these resources would be welcomed. Please email: LTLC@hee.nhs.uk.
-
Complete courses
Complete courses: Simulation scenario-based programmes
- COVID Preparation Course, Level 2 & Level 3 Patient Care – 2 Day Programme
- COVID-19 redeployed staff Critical Care training programme
- Training programme for redeployed staff in Critical Care: COVID 19
- ICU Cross-skilling course for Redeployed Staff A-E course
- NWL Surge Tracheostomy Training
- COVID-19 On the Wards: Remote video debriefing course
Complete courses: Other
-
Field hospital resources
London Field Hospital Resources
- Overview documents
- Red Training programme
- Amber Training programme
- Green Training programme
- Purple Training programme
- Day Zero
- Posters
- Simuation Scenarios
Yorkshire & Humber Field Hospital Resources
-
Simulation and human factors guides
-
Digital and remote teaching skills
-
Clinical guidance (2020)
-
Lesson plans
-
Instructional videos
-
Publications and webpages
-
Slide deck
Managing the COVID-19 surge: 10 quick wins for ICUs
Frontline clinicians working with the National Clinically-Led workforcE and Activity Redesign (CLEAR) Programme for ICU, as part of the LTLC, are sharing 10 recommendations that can be adopted in ICU in 48 hours. While working collaboratively across 4 London trusts, clinicians identified these “quick wins” in response to the experience and reflections of staff in the first wave of the pandemic.
-
Managing the COVID surge: 10 quick wins for ICUs
Managing the COVID surge: 10 quick wins for ICUs
The National CLEAR Programme provides training, data analytics and modelling tools for Clinically-Led workforcE and Activity Redesign (CLEAR). CLEAR participants working in ICUs across 4 London trusts have identified ‘quick wins’ to share with colleagues across the NHS. Whilst these recommendations may seem straightforward and ‘common sense’, our evidence shows that they improve communication, staff wellbeing and patient care.
All of the recommendations can be adopted within 48 hours. The 10 Quick Wins infographic (PDF, 1125KB) provides a summary checklist for discussion in multi-disciplinary planning forums and staff meetings. Download the printer ready version (PDF, 295KB). The 10 Quick Wins slidedeck (PDF, 820KB) provides further details and practical examples.
Research outputs informing our programme
-
Learning from the education experiences of ICU staff (survey)
The LTLC have surveyed almost 1000 ICU staff from across London in order to understand their experiences of education during the COVID pandemic. This includes critical care educators, critical care staff who received education and staff redeployed to ICU. The feedback that has been received from across London is informing the work of the LTLC, including the co-development of the skills matrix and the collation of resources.
Summary of results
Please find below summaries of the survey results broken down by group:
- ITU staff who primarily delivered education (PDF, 790KB)
- ITU staff who primarily received education (PDF, 391KB)
- Redeployed nursing staff (PDF, 1061KB)
- Redeployed occupational therapists (PDF, 794KB)
- Redeployed speech and language therapists (Microsoft PowerPoint, 428KB)
- Redeployed Dieticians (PDF, 1490KB)
- Redeployed Physiotherapists (PDF, 1174KB)
- Redeployed Doctors (Microsoft PowerPoint, 445KB)
- Healthcare Assistants (PDF, 1454KB)
- Redeployed healthcare scientists (Microsoft PowerPoint, 423KB)
- Redeployed Pharmacists (Microsoft PowerPoint, 406KB)
- Other redeployed staff groups (PDF, 1232KB) including operating department practitioners dentists/dental assistants and nurses, students, podiatrists, midwifes, nursing associates and advanced clinical practitioners
-
A survey into the workforce utilised to support critical care units during COVID-19
Two short surveys were developed in collaboration between the Intensive Care Society (ICS) and the Operational Delivery Network (ODN) representatives, and disseminated via Survey Monkey over the month of May 2020. One was specifically for critical care managers/nurse leads to complete, the other for staff who were redeployed into critical care.
The aims of the surveys were to obtain a snapshot of the additional workforce mobilised to manage critical care surge during the COVID-19 crisis. The aim was that that the data returned can help inform areas of good practice, and identify areas for improvement in future, should the need for staff redeployment to critical care be required again.
Download the results of the survey (PDF, 885KB).
-
LTLC emerging findings: changes to models of care on ICU (infographic)
Results from a rapid qualitative appraisal based on telephone interviews with staff across ICUs in London to:
- document changes made it ICU models of care
- explore challenges and enablers in the implementation of these changes
- identify the aspects of care delivery that worked well and areas for improvement
Download the infographic (PDF, 6460KB).
-
NHS staff experiences of working in critical care – The CLAP Study (infographic)
Results of telephone interviews with 40 staff from critical care units in Scotland and England.
Download the infographic (PDF, 1527KB).
Additional materials
-
FICM and HEE Skills Passport
“The entire intensive care community is keen to acknowledge the contributions made during the COVID-19 pandemic by many members of the multidisciplinary team (MDT). In particular, those who were deployed into Critical Care areas, joined rotas, used existing skills, and cross-skilled as abilities and supervision permitted.
The Faculty understands that for medical trainees, nurses and Allied Health Professionals (AHPs) who do not generally work in Critical Care, getting recognition for any new or added ICM skills obtained during the pandemic can be problematic. In conjunction with Health Education England (HEE), we have developed a ‘COVID Passport’ to help those individuals get the recognition they deserve.
The Passport is comprised of two sections:
- Care Packs: Each ‘Care Pack’ contains examples of skills and work undertaken during deployment to Critical Care that individuals can denote that they have completed. This section is counter-signed by a supervisor in ICM (this may be a consultant, charge nurse, senior AHP or line manager, as appropriate) to certify that the health professional has worked in these general areas to the denoted level of supervision.
- Skills Self-Certification: Specific skills developed can be delineated further, in the ‘COVID-19 Skills Passport Clarification’ section of the document. This will provide future employers and trainers with more detail on individual attainments. Please note that this section is entirely self-certified and is not signed-off by an ICM supervisor.”
-
Delivering oxygen therapies
This resource (PDF, 6.6MB) was designed as a high-level document to highlight the risks of a catastrophic event relating to oxygen use, limited supplies and failure. The following topics are covered:
- Catastrophic oxygen failure and mitigating the risks
- Oxygen consumption and good housekeeping guidance
- Risk of fire and mitigating actions
This resource is designed for all clinical staff working in areas delivering oxygen therapies. This document does not present any original guidance; national and regional guidance has been collated where appropriate. All guidelines used are referenced and linked in the relevant sections. This document is correct at the time of construction (January 2021); however, please be aware that specific guidelines may change with time.











